Weight Loss Surgery
In many respects, Janet was just like any other 26 year old. She had a stable job, she enjoyed her leisure time with friends, family and two dogs, and she was keen to find a special someone to date.
Janet however, was not like everyone else in one respect, Janet was morbidly obese. Her ideal weight according to the Body Mass Index (BMI) was almost half her 319 pounds. She had trouble finding clothes that fit, and felt uncomfortable going out with friends. While she had dreams of travel, she was unable to comfortably fit into seats on planes, buses or even behind the steering wheel in her own car.
RELATED ARTICLES
- Tummy Tuck After Weight Loss
- How To Tighten Loose Skin
- Arm Lift Cosmetic Surgery
- Body Lift Surgery
- Thigh Lift Surgery
Janet was also starting the see the effects of her weight in the decline of her health. Her doctors diagnosed the onset of diabetes.
Janet had become one of the increasing number of people in the United States with an obesity problem. Over half the population of the United States is overweight, and a third of the population being classed as obese.
Along with obesity comes a number of health issues that can be fatal, including heart disease, diabetes, some forms of cancer and strokes. The treatment and management of these conditions can be quite distressing, painful and expensive. Estimates on the national annual cost of treating obesity related diseases comes in at around 200 billion dollars per year.
The numbers and consequences of having such a high percentage of our population being obese has become a matter of national concern. Programs have been implemented nationwide to educate children in areas of physical activity, health and nutrition.
Many employers, schools and insurers have implemented wellness programs to assist American's in adopting a healthy lifestyle. Unfortunately for those who are already obese, it is extremely difficult to lose weight without assistance.
 Janet before Gastric Sleeve Surgery, she is 319 pounds.
Janet before Gastric Sleeve Surgery, she is 319 pounds.
Bariatric Surgery
Fortunately for Janet and many others like her, there are now a number of options in bariatric (weight loss) surgery.
Weight loss surgery is an option open to people who despite making concerted efforts, have extreme difficulty in losing weight. As an obese person, there are a number of physical, health and psychological conditions that must be met before undertaking surgery.
While each surgeon will have their own specific conditions, as a general rule patients need to have a BMI over 40, have demonstrated through their previous efforts and psychological assessment, the desire to change their lifestyle to a healthier one and have made efforts through traditional means to lose weight.
In some circumstances, where a person has a obesity related condition such as severe joint pain, diabetes or heart disease, the minimum BMI to be considered as a weight loss surgery candidate can be reduced to 35.
Prior to Surgery
The process for preparation for surgery can be an extensive one. Potential patients undergo numerous interviews to determine their suitability. The surgeon will assess their physical suitability, and counsellors and mental health specialists assess the patient’s readiness to make significant changes and manage the stress of necessary changes once the surgery is completed.
After meeting with your surgeon, together you will make the decision about what procedure would be best for you. Often patients will be put on a prescribed diet and exercise regime. Sometimes, patients who are particularly successful then decide not to continue with surgery. Make sure you speak with your surgeon and insurance company as to their policies regarding patients who drop below the required BMI. While most will still complete the surgery, not all do.
It’s also important to note that weight loss surgery is not a quick fix. Patients need to commit to long term, or lifetime changes to their whole lives including what they eat, and how they move (exercise) before undergoing surgery.
Types of Weight Loss Surgery
When looking into the possibility of weight loss through surgery, there are a number of different options. The three most common of these are Lap banding, Gastric sleeve surgery, and Gastric bypass surgery.
Gastric Bypass
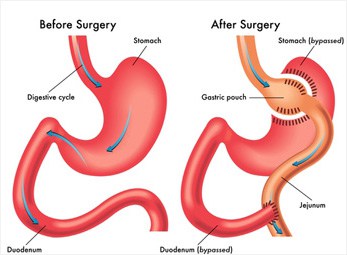
The most common form of weight loss surgery performed world wide, gastric bypass surgery diverts the pathway of the gastrointestinal tract.
Process
A gastric bypass involves a surgeon dividing the stomach and attaching it to the small intestine, creating a much smaller stomach. The dramatically decreased size of the stomach ensures the patient is unable to absorb as many calories, and effects the physiological system of the patient to release different hormones when eating. This often causes the patient to feel full more quickly and for longer.
Success
Gastric bypass surgery usually results in a 50 – 75% loss of excess body weight over two years. Around 70 – 75% of that is lost in the first year alone.
Lap Banding
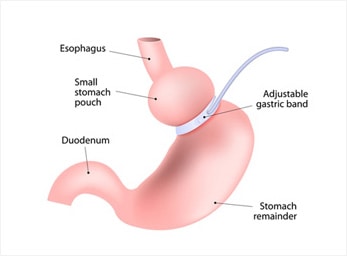
Lap banding is a reversible procedure which involves reduction the size of the stomach, so less food can pass through.
Process
Lap banding or Laparoscopic adjustable gastric banding is a process by which a surgeon inserts a band to reduce the amount of food the patient can eat. It is done using laparoscopy and gives the surgeon the option to adjust the tightness of the band according the patient’s needs. It is a relatively simple operation with a short recovery period, and has the option of being reversible.
Success
Patients undertaking Lap Banding can look forward to a loss of 50 -60% of their excess body weight within the first two years. This depends on the patient’s ability to adhere to the dietary guidelines set by the surgeon and nutritionist before surgery. The surgery will not result in significant weight loss if the patient continues to consume large amounts of calories in a liquid format.
Gastric Sleeve
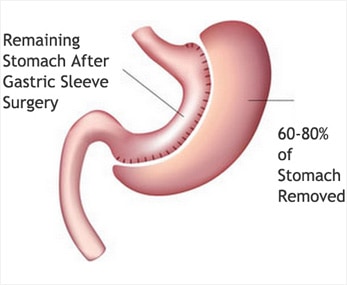
Gastric sleeve is done by surgically removing part of the stomach reducing its size and ability to hold food.
Process
Gastric sleeve or sleeve gastrectomy surgery, involves reducing the size of the stomach to a small tube, roughly the shape and size of a banana. This drastically reduces the amount of food that can be in the stomach at one time, while keeping the integrity of the digestive system. This process allows for the removal of excess stomach and doesn’t divert the food though an unnatural pathway.
Success
After two years, people who have had the surgery completed generally have lost 60 – 65% of their excess body weight. They usually have less issues with malnutrition as their digestive tract is working in the same way as previous to surgery and able to absorb the nutrients from food.
Potential Complications
Regardless of the surgery you decide to undertake there are some things that you need to be aware of and be on the lookout for. Potential complications for all three surgeries can include internal bleeding, infection or leaking or blocked bowels. If any of these happen you should immediately call the doctor or hospital. Unfortunately if things go wrong there may be need for further surgery.
There are a number of things that you can do to minimise these risks. Firstly, choose the place where you’ll be having your surgery done carefully. Research the hospitals near you, and choose one where a lot weight loss surgeries are performed. Experienced surgeons are less likely to have complications come up in their patients. Also, check the level of care and follow ups you’re likely to receive after the operation is completed.
As well as choosing your surgeon, and hospital, ensure you follow all the prerequisites for having your surgery done. These could include a certain number of psychological assessments, dietician appointments as well as recommendations, all of which should be adhered to strictly in order to successfully be approved and complete your weight loss surgery. For many, these recommendations include an extremely restricted diet (often liquid) and an intensive exercise regime which can be challenging for those who are morbidly obese.
After Surgery
After you have completed your surgery, it’s very important to schedule and keep regular appointments with surgeons, dieticians and mental health professionals. Follow the diet carefully and try not to deviate from it. Keep up your exercise from when you started before the surgery. Again your doctors and nutritionist will give you an indication of when you can step up the pace. Be very careful not to fall back into your old habits. If you feel yourself slipping, make sure you reach out and make contact with your health professionals, or your friends and family.
So Is Surgery Worth It?
If you’re prepared to put in the work, following instructions, keeping to the diet and exercise, and making sure you don’t get back into bad eating and exercise patterns, yes it’s worth it. Those who are able to access the surgery, can potentially lose three quarters of their excess body fat, getting them down to a point where they can to function at a much more interactive level.
Patients also potentially save money through reducing incidences of obesity related diseases and complications. And often have a renewed confidence in themselves both looking and feeling better.
...Janet
For Janet, having a gastric sleeve surgery has been life altering. After a year, she had lost 90 pounds and her health had improved dramatically. Her diabetes was stabilised, and she was having less trouble with her back and knees.
Janet’s whole outlook has changed “I feel more comfortable in my own skin, like I have the confidence to go out and meet people, and not always be worried about how I look and what they’re looking at.”
Janet has tried on new clothes, has travelled on busses and comfortably fits behind the wheel of her car. All things that she was struggling with prior to the surgery.
Perhaps most excitingly, she has booked a holiday to Europe in 6 months time when she hopes to have reached her target weight within her healthy BMI range.